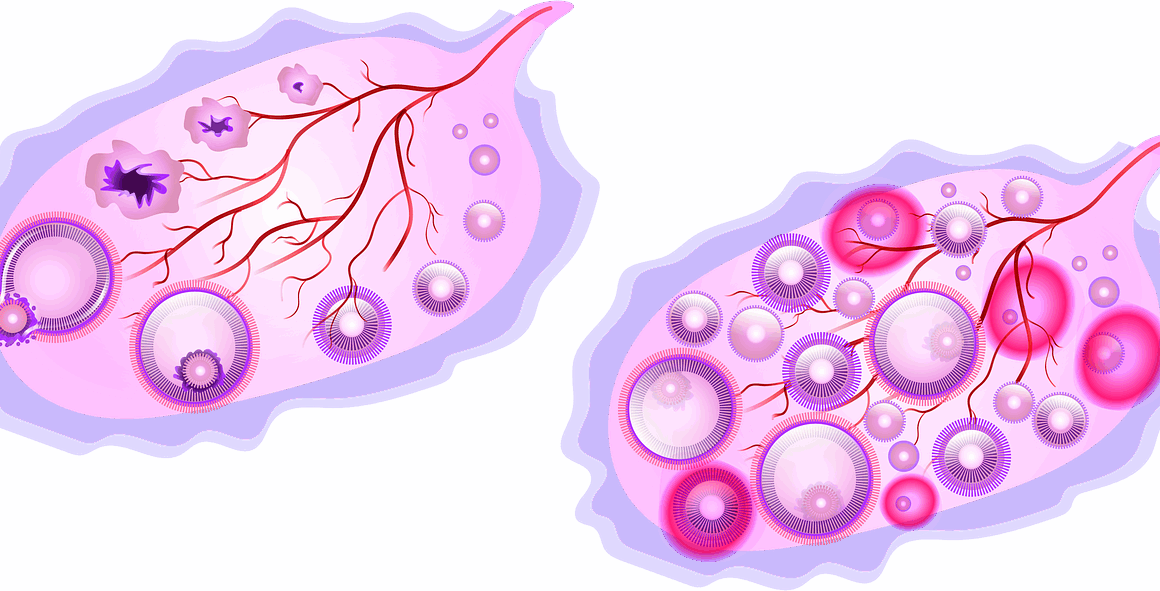
The Effect of Polycystic Ovary Syndrome on Body Composition and Hormones
Polycystic Ovary Syndrome (PCOS) significantly impacts body composition and hormonal balance. Women with PCOS often experience a complex interplay of hormonal imbalances, leading to various physiological changes that affect their overall health. Body composition is crucial as it can determine an individual’s risk for developing more serious health conditions. In fact, the hormonal irregularities in PCOS can contribute to increased fat accumulation, particularly visceral fat, which is associated with metabolic disorders. Furthermore, these women frequently face challenges regarding weight management, as insulin resistance can exacerbate weight gain. This relationship is noteworthy, making the management of body composition critical in PCOS therapy. Lifestyle modifications, including diet and exercise, are often recommended as primary interventions. Research has shown that even small weight reductions can improve hormonal parameters significantly. Additionally, understanding how PCOS alters fat distribution is vital. It is known that fat distribution can contribute to severity of the symptoms experienced by affected women. The necessity for tailored approaches in addressing body composition and hormone levels in PCOS patients cannot be overemphasized, as it provides a pathway toward improving overall health outcomes and quality of life.
The symptoms of PCOS are diverse and can greatly interfere with a woman’s body composition. These typically include irregular menstrual cycles, excessive hair growth, acne, and weight gain. The underlying cause of PCOS involves a combination of genetic, environmental, and hormonal factors. Moreover, hormone fluctuations can lead to increased levels of androgens—specifically testosterone. This hormonal imbalance often manifests as changes in body fat distribution and muscle mass. For instance, women may notice an increase in abdominal fat as opposed to subcutaneous fat, which raises the risk of cardiovascular diseases. Understanding this aspect of PCOS is essential, as it underscores the need for effective body composition strategies. Studies indicate that addressing the hormonal picture through both medication and lifestyle changes can vastly improve body composition metrics. Such measures may include regular exercise regimens and dietary modifications designed to promote metabolic health. Consultation with healthcare professionals specialized in endocrinology can provide tailored treatment options. Awareness about the links between PCOS symptoms, hormonal changes, and body composition should be heightened, thereby empowering women to take action for managing their conditions proactively.
Insulin Resistance and Body Composition
Insulin resistance is a prevalent issue among women diagnosed with PCOS, which directly influences body composition. When insulin resistance occurs, it leads to higher circulating insulin levels in the bloodstream, which can promote fat deposition and hinder weight loss efforts. This increased insulin can also cause the ovaries to produce more androgens, perpetuating the cycle of hormonal imbalances. The result is often a higher percentage of body fat, specifically visceral fat, which poses additional health risks. Various studies have demonstrated a strong correlation between high insulin levels and obesity in women with PCOS, highlighting the critical role of managing insulin sensitivity. Effective management might include adopting a low glycemic index diet, engaging in regular physical activity, and, in some cases, using medications like Metformin that enhance insulin sensitivity. These interventions can be life-changing and are essential for improving not only body composition but overall metabolic health. Women’s health specialists often emphasize these strategies to help patients minimize the effects of PCOS on their body composition and mitigate the associated health risks.
Meanwhile, it is essential to understand that body composition changes in PCOS may not solely stem from weight gain. Women may also experience alterations in lean body mass due to hormonal fluctuations. Lowered muscle mass can negatively affect metabolic rate, creating further challenges in weight management. It’s vital to incorporate strength training exercises that can help build lean muscle, as they contribute positively to overall body composition. Resistance training enhances muscle growth and can improve insulin sensitivity, proving beneficial for women navigating the challenges associated with PCOS. Nutrition, complemented by exercise, plays a significant role in managing body composition. A balanced diet rich in lean proteins, healthy fats, and whole grains can help address issues associated with weight and hormonal balance. Choosing nutrient-dense foods not only assists in achieving and maintaining a healthy weight but also ensures that women receive the essential nutrients necessary for managing their hormonal health. In most cases, implementing such strategies can significantly improve body composition parameters, leading to far-reaching benefits within the scope of PCOS management.
The Role of Diet in Hormonal Balance
Diet plays a crucial role in regulating hormonal balance and, subsequently, body composition in women with PCOS. Implementing a more balanced diet is often the first recommended approach to managing symptoms related to the syndrome. Foods that are high in processed sugars and unhealthy fats should be limited, as they can exacerbate insulin resistance and lead to weight gain. Instead, diets focused on whole foods—such as fruits, vegetables, whole grains, and lean proteins—have been shown to support hormonal stability and regulate body composition. Specific dietary plans, such as the Mediterranean diet, have been widely recognized for their benefits in reducing inflammation and promoting hormonal health among PCOS patients. Alongside dietary adjustments, it is recommended that women with PCOS stay consistent with meal timing and portion sizes to optimize caloric intake. Many women report improvement in symptoms and metabolic markers within a few months of making these changes in their diets. However, it’s vital to tailor dietary recommendations to individual needs and preferences, ensuring sustainable lifestyle changes. This approach not only addresses PCOS symptoms effectively but can also promote a healthier weight and better body composition.
Exercise is another cornerstone in managing PCOS and improving body composition. Regular physical activity directly influences body weight, composition, and metabolic function. Exercises such as aerobics and resistance training have been shown to enhance insulin sensitivity, thereby assisting women in managing their weight effectively. Additionally, exercise can lead to reductions in visceral fat, which is particularly harmful and linked with various metabolic syndromes. Beyond physical changes, engaging in regular exercise can also improve mood and reduce the risk of anxiety and depression, which are prevalent among women with PCOS. It is recommended that women engage in at least 150 minutes of moderate-intensity aerobic exercise weekly, alongside strength training exercises twice a week. Finding enjoyable methods of staying active can contribute significantly to adherence and success in exercise regimens. Collaborating with fitness professionals who understand the unique challenges of PCOS can further enhance the effectiveness of exercise programs, making them personalized to each individual’s capabilities. Collectively, incorporating a dedicated exercise routine can dramatically alter both body composition and hormonal health, resulting in an overall positive outlook.
Conclusion and Actionable Steps
In conclusion, understanding the complex interplay between body composition and hormonal effects in women with PCOS is essential for empowering effective management strategies. This condition presents a unique set of challenges, primarily through hormonal imbalances leading to alterations in body fat distribution and metabolism. Engaging in a multifaceted approach that includes dietary modifications, exercise, and regular monitoring of body composition is key. Women should be proactive in seeking individualized treatment plans and regularly communicate with healthcare providers to monitor changes effectively. Employing these strategies contributes not only to improving body composition but also enhances overall quality of life. Furthermore, raising awareness about PCOS among healthcare professionals and the general public can foster understanding and support for affected women. With adequate knowledge and resources, women with PCOS can make informed choices, paving the way toward better health outcomes. In doing so, they can combat the effects of PCOS more successfully, improving their health picture and achieving a better sense of well-being. Initiating this journey may be challenging, but the potential rewards are substantial for women navigating the world with PCOS.
In summary, the implications of PCOS on body composition and hormonal health are profound and demand attention. Women diagnosed with PCOS need to embrace a proactive approach toward managing their symptoms and understanding their health. The integration of healthy living strategies, including diet, exercise, and emotional support, can lead to significant improvements. Knowing the importance of body composition in relation to hormonal health can stimulate essential dialogue among healthcare providers and patients alike. The key takeaway is that with the right plan in action, managing PCOS is entirely possible. Factors such as insulin resistance, dietary choices, and exercise regimens all play integral roles in shaping the body composition of women dealing with PCOS. Moreover, developing a supportive community and fostering resilience can contribute to tackling challenges faced in this journey. Therefore, the future looks brighter for women affected by PCOS as awareness grows and effective management strategies are established. Navigating this condition offers the opportunity for personal growth and improved health, reinforcing the message that change is possible and that support is available.