Effect of Menopause on Hormones and Bone Health
Menopause is a significant transition in a woman’s life that can dramatically affect hormonal levels and bone health. This change typically occurs between ages 45 and 55, marking the end of menstruation and a decline in ovarian function. The decrease in estrogen, a crucial hormone for maintaining bone density, directly influences the structure and integrity of bones. Lower estrogen levels lead to increased bone resorption, which means that the body loses bone density faster than it can create new bone. Consequently, the risk of osteoporosis rises significantly. Osteoporosis is a condition characterized by weak and fragile bones that can lead to fractures even from minimal stress. Research shows that postmenopausal women have a much higher risk of developing osteoporosis compared to premenopausal women. Additionally, the hormonal changes can also lead to a host of other health issues, including cardiovascular disease and metabolic disorders, which further complicate the health picture for postmenopausal women. Regular monitoring of bone health and hormone levels during this transition can help in employing preventative measures, improving overall quality of life.
During menopause, women often experience varying physical and emotional symptoms due to hormonal fluctuations. These symptoms can include hot flashes, night sweats, mood swings, and vaginal dryness. All these changes can impact a woman’s quality of life and mental well-being. Furthermore, hormonal changes during this period result in various bodily transformations, including alterations in metabolism and body fat distribution. Estrogen, which plays a vital role in maintaining physical and emotional health, decreases significantly, leading to negative physical changes. Consequently, these changes may encourage sedentary behavior due to discomfort, exacerbating the decline in bone health. It is crucial for women to understand these symptoms and recognize that weight-bearing exercises become increasingly important during menopause. Activities such as walking, weightlifting, and dancing can help improve bone density. Seeking professional guidance from healthcare providers can also ensure women tailor their exercise routines appropriately to meet their individual needs and comfort levels. This knowledge empowers women to take control of their hormonal health and make informed decisions regarding their fitness during this transitional period. Incorporating lifestyle changes can mitigate adverse effects and enhance overall health.
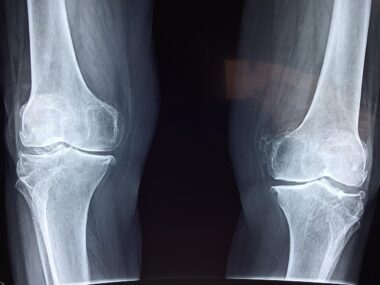
Impact on Bone Density
The impact of menopause on bone density cannot be overstated, as the postmenopausal period witnesses a rapid decline in bone density. Osteoporosis develops when the rate of bone resorption exceeds the rate of bone formation, creating an imbalance. As estrogen levels plummet, the body’s ability to rebuild bone is impaired, leaving bones more porous and fragile. Studies reveal that women can lose up to 20% of their bone density within the first five to seven years post-menopause. It’s crucial to conduct regular bone density screenings during this time to identify any loss early on. Early detection can facilitate interventions that include nutritional supplements, dietary changes, and prescribed medications to mitigate future risks. Calcium and vitamin D intake play a significant role in maintaining bone strength during this time. Women must ensure an adequate intake of these nutrients from their diet or supplements. In addition, lifestyle choices such as minimizing smoking and limiting alcohol consumption can positively affect bone health. Collaborative efforts with healthcare professionals can provide tailored guidance on monitoring bone health and implementing effective prevention strategies.
Nutrition plays an essential role in supporting bone health, particularly during menopause. A well-balanced diet rich in calcium, vitamin D, and other key nutrients is fundamental for maintaining bone density after menopause. Calcium is necessary for bone structure, while vitamin D aids calcium absorption in the body. Women should consider integrating various calcium-rich foods, including dairy products, leafy greens, fortified foods, and fish, into their diets. Vitamin D, on the other hand, can be obtained from sunlight exposure, fatty fish, and fortified foods. In addition to calcium and vitamin D, magnesium, phosphorus, and potassium are also crucial for bone maintenance. Furthermore, a diet low in processed foods and high in fruits, vegetables, lean proteins, and whole grains can significantly enhance overall health during menopause. Hydration also plays a pivotal role in maintaining bodily functions and supporting metabolic processes. Women should focus on incorporating healthy fats from sources like nuts and avocados, which can have a beneficial effect on hormone levels and overall wellness. Personalized nutritional plans can provide guidance and recommendations that suit each individual’s dietary needs. Consulting with a nutritionist can further enhance this aspect of health management.
Exercise and Physical Activity
Engaging in regular physical activity is vital for preserving bone health in postmenopausal women. Weight-bearing exercises, such as running, walking, and resistance training, are particularly beneficial. These types of workouts exert force on the bones, stimulating bone growth and strengthening the skeletal system. Incorporating a variety of exercises can also help address different aspects of fitness. Balance and flexibility exercises, like yoga or tai chi, not only enhance physical stability but also aid in reducing the risk of falls, which can lead to fractures. In addition, aerobic activities benefit cardiovascular health and can improve overall mood and mental well-being. Adequate physical activity can mitigate some menopausal symptoms, including anxiety and depression, by releasing endorphins that foster a sense of well-being. It is essential for women to create an exercise routine that they genuinely enjoy, as this increases adherence and long-term success. Working with fitness professionals can establish safe programs tailored to individual capabilities, preferences, and any existing health issues. This multifaceted approach can significantly enhance women’s health outcomes during and after menopause.
Identifying the signs of hormonal changes during menopause is paramount for taking proactive measures to safeguard bone health. Women should be aware of their bodies and take note of any significant changes they experience physically and emotionally. Tracking menstrual cycles and any irregularities may provide insight into impending menopausal transitions. Regular check-ups with healthcare providers can lead to discussions surrounding hormonal testing and possible therapies, such as hormone replacement therapy (HRT). HRT can help reconcile the fluctuations in hormone levels and may reduce bone loss significantly. Conversely, it is essential to weigh the risks and benefits of HRT, as it might not be suitable for everyone. Women must have informed discussions with their healthcare providers regarding family history and personal health histories to make appropriate decisions about HRT. In addition, understanding genetic predispositions can help identify risks associated with osteoporosis. Educating oneself about hormone levels, symptoms to monitor, and the importance of routine screenings can significantly empower women regarding their health management. Increased awareness fosters informed decisions that enhance overall quality of life during this critical transition period.
Conclusion and Future Directions
In conclusion, menopause brings significant hormonal changes that directly impact bone health and overall well-being. Women must engage in active management of their health throughout this life stage by prioritizing lifestyle adjustments that can mitigate risks associated with this transition. Awareness of the signs and symptoms of menopausal changes, combined with proactive approaches like diet, exercise, and regular medical consultations, can promote better health outcomes. In the future, continued research into hormone therapies and innovative treatment modalities may provide additional strategies to support women during menopause. There is potential for developing personalized treatment plans tailored to individual needs, providing more robust support for managing menopause effectively. Furthermore, public health initiatives can raise awareness about the importance of hormonal health and its implications for bone health during this life stage. Collaboration between healthcare professionals, researchers, and communities will be essential in providing the resources, education, and support necessary for women approaching menopause. By actively prioritizing their health, women can enjoy a fulfilling and healthy postmenopausal life, minimizing the adverse effects of hormonal changes and maintaining bone strength.
Improved lifestyle choices and preventive measures can help women manage the effect of menopause on hormonal health. Fostering a supportive environment that encourages women to share their experiences, challenges, and solutions can improve overall understanding of menopause. This, in turn, can lead to stronger social networks that provide emotional support crucial during this transition. Increased education and awareness can bridge gaps in knowledge regarding the significance of hormonal health in relation to lifestyle factors. Moreover, integrating community resources such as wellness programs focused on fitness and nutrition may help empower women to prioritize their health. Multidisciplinary approaches can also offer comprehensive care that addresses the biological, psychological, and social factors influencing women during menopause. Embracing technological advancements in health monitoring devices can enhance self-management of health and wellness. Encouraging women to engage in forums, workshops, and online platforms focused on menopause health can generate a wealth of shared knowledge. Overall, a collective effort toward supporting women’s hormonal health will enhance their ability to lead healthy, active lives as they navigate the challenges and changes associated with menopause.