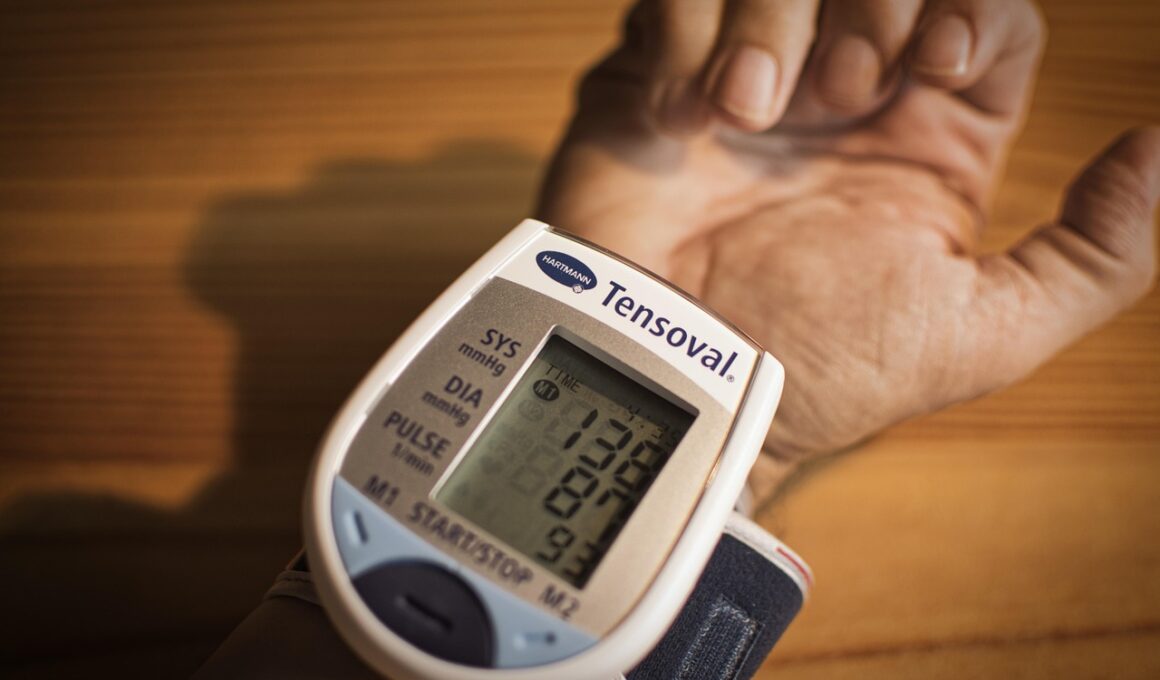
Intermittent Fasting Effects on Systolic and Diastolic Blood Pressure
Intermittent fasting has gained popularity as a health strategy among various diet enthusiasts. Many people explore intermittent fasting due to its potential benefits, particularly on metabolic health. Numerous studies indicate that fasting can yield significant improvements in blood pressure levels, leading to enhanced cardiovascular health. Hypertension is a common health issue that affects millions of people worldwide. Evidence suggests that intermittent fasting may help manage both systolic and diastolic blood pressure effectively. Various forms of fasting exist, such as a 16/8 method, where individuals restrict their meals to an eight-hour window. This approach may reduce overall calorie intake, postulated to reduce blood pressure significantly. Fasting can also improve insulin sensitivity, leading to better glycemic control and lower blood pressure readings. Researchers have observed that the process of fasting might influence neurohormonal systems that regulate blood pressure. However, individual responses can vary, and it’s essential to consult healthcare providers, especially for those on medication. Incorporating intermittent fasting may provide feasible solutions for individuals struggling with hypertension and maintain better overall health.
Mechanisms of Action
The potential mechanisms through which intermittent fasting affects blood pressure are multi-faceted and complex. One key mechanism involves the reduction of inflammation in the body, which is closely linked to chronic diseases, including hypertension. By decreasing inflammatory markers, fasting may lead to improved blood vessel function. This effect encourages vasodilation, allowing blood to flow more freely and reducing overall pressure on arterial walls. Fasting can also regulate certain hormonal levels that help maintain cardiovascular stability. For example, during fasting, levels of norepinephrine may increase, leading to improved heart performance and blood pressure regulation. Moreover, caloric restriction combined with fasting influences the renin-angiotensin-aldosterone system, crucial for blood pressure regulation. Another notable point is that fasting promotes a state of autophagy, where the body cleans out damaged cells and regenerates healthier cell populations. Such cellular renewal can enhance cardiac functions over time. These combined effects make intermittent fasting a practical approach for individuals aiming to manage blood pressure more effectively while promoting overall health. Further research is essential to clarify these mechanisms fully and their implications for long-term health.
Several studies have reported promising results regarding intermittent fasting’s impact on systolic and diastolic blood pressure. Research conducted on various populations consistently shows that participants undertaking intermittent fasting regimens experience a reduction in both systolic and diastolic values. A systematic review highlighted the need for more extensive trials to determine optimal fasting duration and schedules across different demographics. Various durations of fasting demonstrate differing outcomes. For instance, a study focusing on alternate-day fasting indicated significant blood pressure reductions among participants at risk of hypertension. Notably, lifestyle factors play a crucial role in individual results, such as diet quality and physical activity. Integrating a balanced diet rich in fruits, vegetables, whole grains, and lean proteins while practicing intermittent fasting may enhance its effects on blood pressure regulation. Those following higher caloric intake during eating windows might not experience the same benefits. Additionally, maintaining hydration is vital during fasting periods to support cardiovascular health. It is essential to consider personalized approaches that consider individual preferences and health conditions to optimize outcomes effectively.
While intermittent fasting presents several advantages for blood pressure management, it’s crucial to acknowledge possible challenges and risks. Individuals with existing health conditions, such as heart disease or diabetes, should consult healthcare professionals before starting a fasting regimen. Moreover, people taking medications that affect blood pressure must also consider their regimen’s timing with meals. Certain fasting methods may not be suitable for everyone. For example, longer fasting durations could lead to fatigue, dizziness, or other adverse effects. Adapting fasting approaches to individual needs is crucial for success. Some individuals may find adopting a more flexible eating plan beneficial, providing structure without severe restrictions. Incorporating mindfulness and self-monitoring techniques can help maintain adherence and positively influence blood sugar levels. Furthermore, families and individuals should consider incorporating physical activity that complements intermittent fasting for improved results. Light to moderate exercise enhances overall health and blood pressure regulation, providing additional benefits when combined with fasting. The interplay between nutrition, exercise, and fasting can create a balanced life that supports optimal blood pressure management and improved overall well-being.
Real-World Applications
Implementing intermittent fasting as a practical strategy for managing blood pressure requires thoughtful consideration and planning. Setting realistic fasting goals and ensuring adequate support systems can enhance adherence to the practice. Individuals may benefit from tracking their fasting schedules, food intake, and blood pressure measurements to monitor progress. This process empowers users and helps identify potential areas for improvement. Joining groups that support intermittent fasting can foster community connections, sharing success stories, and tips, providing motivation throughout the journey. Integrating intermittent fasting with a well-balanced diet and exercise routine significantly enhances its effectiveness. Nutrition plays a vital role; focusing on nutrient-dense foods ensures the body receives essential vitamins and minerals during eating windows. Establishing proper meal timing, choosing the right types of foods, and portion control can yield weight loss and blood pressure improvement. For many individuals, making gradual lifestyle changes over time leads to greater long-term success compared to drastic dietary adjustments. This gradual approach encourages the adoption of healthier habits, making fasting a sustainable long-term solution for blood pressure management and general health improvement.
Concisely, intermittent fasting presents a compelling approach for individuals seeking to manage blood pressure levels. The substantial evidence supporting intermittent fasting’s potential benefits provides an incentive to explore this dietary strategy as an option for improving cardiovascular health. However, certain factors must be acknowledged to maximize the advantages of fasting effectively. Adapting to various approaches, understanding individual health conditions, and recognizing emerging scientific insights are essential for success. Those considering such an approach should take the time to educate themselves on intermittent fasting types and health benefits. Practical knowledge enables individuals to assess their lifestyle while seeking ways to incorporate fasting sustainably. Establishing a balance between fasting, nutrition, hydration, and physical activity fosters experiments yielding favorable outcomes. Ultimately, individuals must prioritize their well-being throughout the fasting process, leading to lasting improvements. As research continues to unfold the effects of intermittent fasting on hypertension, staying informed will ensure individuals utilize the best strategies for their health needs. Embracing intermittent fasting can be a step towards not only better blood pressure management but also a holistic approach to overall health and wellness.
Conclusion and Future Directions
In conclusion, intermittent fasting demonstrates significant promise in the management of blood pressure and cardiovascular health. Continued research into the intricacies of intermittent fasting will be critical in identifying best practices for various populations. Understanding how different fasting methods influence individual health outcomes can guide recommendations. Moreover, the potential for personalized fasting plans can significantly enhance effectiveness, customizing approaches to meet unique needs. Individuals aiming to lower blood pressure may benefit from integrating fasting with their existing healthcare regime, leading to positive changes. Collaborative approaches with nutritionists or health coaches offer additional pathways for support, ensuring that individuals can embark on their fasting journey with confidence. Raising awareness about the relationship between intermittent fasting and hypertension can help individuals recognize alternatives for managing their health proactively. As knowledge expands, individuals will have access to growing tools and strategies that promote long-term health. This continued evolution in research is vital, providing a deeper understanding of dietary practices and their broad ramifications on health and well-being. Finding the right balance through intermittent fasting may lead to regulatory benefits in blood pressure and overall enhanced quality of life for many.
Ultimately, understanding the role of intermittent fasting in blood pressure management is a significant leap towards a comprehensive health journey. By examining the current landscape of research and future directions, individuals can harness the power of fasting to improve their health. Engaging with healthcare providers and tailoring individual plans ensures adherence to intermittent fasting. Focus should be placed on creating a supportive environment, fostering better health outcomes, and encouraging positive modifications. Maintaining an outlook of hope and curiosity may encourage individuals to explore intermittent fasting deeper. As new evidence emerges, individuals can adapt their strategies according to best nutritional practices and personal health goals. By prioritizing health through informed choices and sustainable methods, further advancements may enhance cardiac health. Additionally, fostering community through shared knowledge and experiences can lead to improved adherence and success stories. Awareness campaigns can effectively amplify the message surrounding the benefits of intermittent fasting. It contributes to achieving healthier lifestyles and robust cardiovascular systems. Overall, embracing science and collaboration fosters promising futures for hypertension management, highlighting the evolution of dietary interventions and their potential impacts.