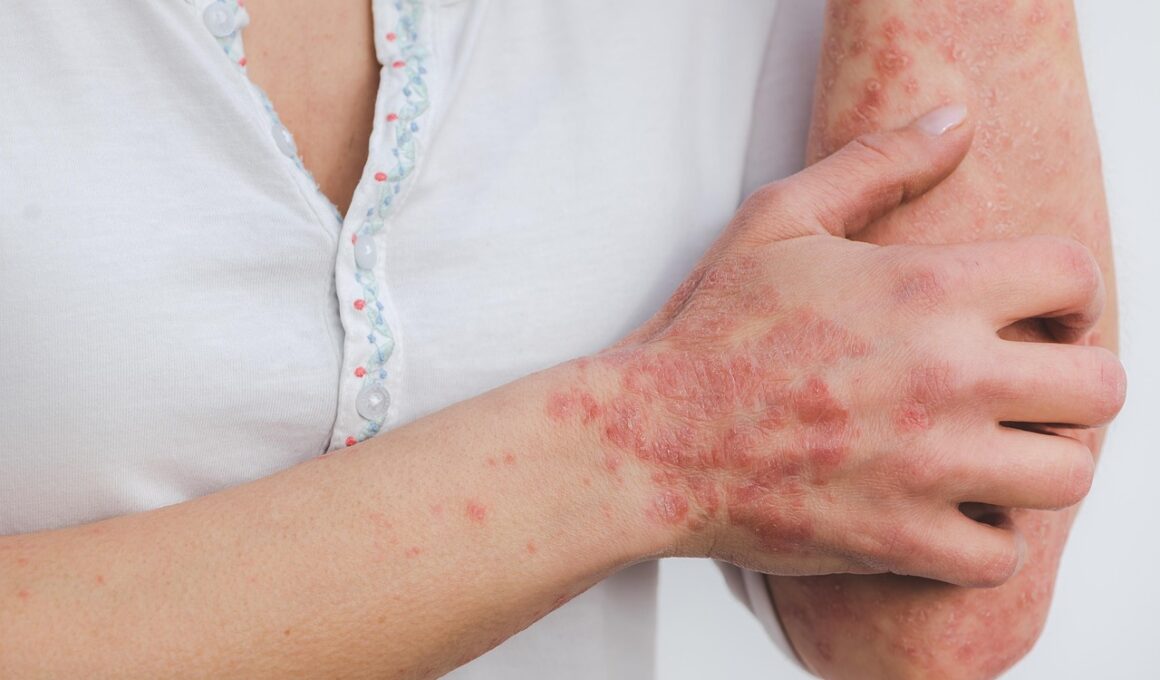
Hormonal Imbalance and Its Role in Autoimmune Skin Diseases
Hormonal imbalance can significantly impact various bodily processes, including immune responses. This disruption often leads to autoimmune diseases, particularly those affecting the skin. Hormones, such as cortisol, estrogen, and thyroid hormones, play crucial roles in regulating inflammation. When these hormones are out of balance, the body’s ability to manage inflammatory responses diminishes, potentially triggering autoimmune conditions. In particular, skin diseases such as psoriasis and lupus exhibit significant associations with hormonal fluctuations. Research suggests that the skin can reflect internal hormonal changes, leading to visible symptoms of autoimmune diseases. It’s critical to recognize the intricate relationship between hormonal levels and immune function. Factors such as stress, diet, and lifestyle can further exacerbate hormonal imbalances. Evaluating these aspects holistically can provide insights into managing autoimmune skin conditions effectively. Furthermore, understanding the role of hormones enables patients and healthcare providers to devise comprehensive treatment strategies. Addressing hormonal health may improve skin conditions and overall quality of life for affected individuals. Consequently, deeper investigation into hormonal health might reveal preventative measures for those at risk for autoimmune skin diseases. Knowledge is empowering when managing health challenges.
The Connection Between Stress and Hormonal Imbalance
Stress is a significant factor contributing to hormonal imbalance. When experiencing chronic stress, the body produces excess cortisol, which can disrupt the normal function of various hormones. This disruption can lead to alterations in immune responses, making individuals more susceptible to autoimmune disorders. Increased cortisol may amplify inflammation, worsening skin conditions linked to autoimmune diseases. Additionally, chronic stress affects other hormone levels, including adrenal hormones, thyroid hormones, and even sex hormones, ultimately impacting skin health and immune function. For example, fluctuating estrogen levels can exacerbate skin issues, such as eczema and psoriasis, especially during hormonal changing life stages like puberty, menstruation, or menopause. Understanding how stress-induced hormonal changes influence skin diseases is essential for developing effective treatment strategies. This knowledge emphasizes the importance of stress management techniques, such as mindfulness, exercise, and relaxation therapies. Implementing proactive lifestyle choices can help regulate hormonal balance, potentially alleviating autoimmune symptoms. Patients should seek guidance from healthcare professionals to design effective stress management plans tailored to their needs. By prioritizing both mental and hormonal health, individuals gain a deeper understanding of the factors contributing to their autoimmune conditions.
Autoimmune skin diseases often manifest differently based on hormonal levels. Conditions like lupus and scleroderma may show varying symptoms in women due to hormonal fluctuations during menstrual cycles. Additionally, hormonal therapies aimed at regulating levels can have significant effects on the management of autoimmune skin conditions. For instance, some patients may benefit from hormone replacement therapy to maintain hormonal balance and alleviate symptoms associated with their diagnosis. However, it’s vital to approach hormone therapy with caution, as it can have side effects and risks. Patients should work closely with specialists who understand the unique intersection of hormonal health and autoimmune diseases. Understanding the specific hormonal interactions at play can help determine appropriate treatments for individuals battling autoimmune skin diseases. In exploring these options, it’s essential to assess lifestyle habits, nutritional choices, and overall health metrics. Combining hormonal management with holistic approaches may yield positive outcomes for patients. Exploring treatments through research and community support helps foster connections between hormone levels and autoimmune skin disease management. Maintaining open communication with healthcare providers is essential to navigate treatment options effectively, enabling individuals to feel empowered by their health journey.
Diet’s Impact on Hormonal Health
Diet plays a crucial role in maintaining hormonal balance, which subsequently influences autoimmune skin disease manifestations. A well-rounded diet rich in whole foods, including vegetables, fruits, lean proteins, and healthy fats, can support endocrine function. Consuming certain nutrients helps regulate hormone levels, thus reducing inflammation and the risk of autoimmune flare-ups. Omega-3 fatty acids, found in fish and nuts, possess anti-inflammatory properties that can benefit individuals suffering from skin-related autoimmune diseases. Additionally, vitamins such as D, C, and E are vital for immune support and skin health. Limiting processed foods and sugars can significantly benefit hormonal balance, as these often lead to inflammation and exacerbate autoimmune symptoms. Staying well-hydrated and avoiding excessive caffeine can also improve hormonal health in individuals with autoimmune conditions. Those looking to improve their symptoms should consult registered dietitians for personalized dietary recommendations. Monitoring food intake and adjusting as necessary can lead to positive results. Ultimately, a balanced diet serves not just to enhance hormonal health but also to uplift overall well-being and quality of life for those suffering from autoimmune skin diseases.
Emerging research continues to shed light on the role of gut health in hormonal regulation and autoimmune diseases. The gut microbiome significantly influences hormone production and immune responses. An imbalance in gut bacteria may contribute to hormonal disruption and exacerbate autoimmune skin conditions. Probiotics and fiber-rich diets can support a healthy gut microbiome, ultimately promoting better hormonal balance. This relationship signifies the importance of addressing gut health alongside hormonal and autoimmune concerns. Exploration into probiotics highlights their potential benefits for individuals diagnosed with autoimmune skin diseases. Studies indicate that specific probiotic strains positively impact hormone production and inflammation levels. As a result, many healthcare professionals advocate incorporating probiotics and fermented foods into daily diets. However, it remains important to consult healthcare providers before starting any supplementation regimen. Understanding how gut health interacts with hormonal health can empower individuals to make informed decisions about their diets and overall wellness. In conclusion, optimizing gut health is vital for managing both hormonal levels and autoimmune skin disease symptoms. This interconnectedness opens the door for innovative approaches, enhancing treatment methods and improving patients’ quality of life.
The Importance of Regular Exercise
Regular exercise is a vital component of maintaining hormonal health and managing autoimmune diseases. Engaging in consistent physical activity helps regulate hormonal levels, reduces stress, and boosts immunity—all critical factors contributing to overall wellness. Exercise releases endorphins, also known as ‘feel-good’ hormones, which can help mitigate stress and inflammation. For individuals with autoimmune skin diseases, participating in low-impact activities encourages circulation and supports skin health. Yoga, swimming, and walking are all excellent exercise options for those experiencing joint pain or skin sensitivities. Establishing a regular exercise routine not only enhances physical fitness but also promotes mental clarity and emotional stability. Combining strength training with cardiovascular activities can further improve hormonal regulation, creating a balanced lifestyle. Acknowledging the importance of movement aids individuals in developing personalized exercise plans that cater to their unique challenges. Ultimately, consistency remains crucial in achieving desired health impacts. Patients should seek guidance from fitness professionals to develop tailored exercise programs suited to their needs. Prioritizing physical activity empowers those with autoimmune skin diseases to take charge of their health and improve their quality of life significantly.
Advancements in research are yielding exciting possibilities for understanding the hormonal connections involved in autoimmune skin diseases. Clinicians and scientists are increasingly recognizing the importance of exploring these intricate relationships. Innovative diagnostic methods aim to assess hormones’ influences on autoimmune conditions more effectively. Innovative testing allows for comprehensive analyses that can unveil the interactions between hormones and immune dysfunction. Additionally, ongoing studies exploring integrative medicine emphasize the holistic approach to treating autoimmune diseases. Incorporating hormonal health management into therapeutic regimens can lead to better patient outcomes. By addressing hormonal imbalances and considering other contributing factors, healthcare providers may develop more effective treatments. This collaborative approach empowers patients with a better understanding of their health and enhances shared decision-making regarding treatment options. Furthermore, future research endeavors will likely reveal additional therapies that focus on normalizing hormones while addressing autoimmune conditions. As the scientific community dives deeper into connection comprehension, we can anticipate advancements in care strategies catering to this intersection. As knowledge evolves, so does the potential for live-improving treatments for individuals affected by autoimmune skin diseases. Ongoing collaboration between researchers and healthcare providers is essential for advancing these inspiring developments.
Conclusion and Future Directions
In summary, understanding hormonal imbalance and its role in autoimmune skin diseases is crucial for improving patient care. Comprehensive knowledge of hormone-immune system interactions highlights the importance of addressing hormonal health. Recognizing stress, diet, gut health, and exercise contributes significantly to managing autoimmune conditions. Collaboration between patients and healthcare providers can lead to more personalized treatment approaches that consider these interconnected factors. Moreover, the evolving research landscape suggests that focusing on hormonal health as part of autoimmune disease management can yield promising outcomes. Future initiatives should continue exploring the intersections of hormonal health and autoimmune disorders. This exploration will empower individuals to make informed decisions about their health, ultimately leading to enhanced quality of life. Furthermore, education plays a pivotal role in raising awareness of hormonal influences on autoimmune conditions across healthcare specialties. Encouraging dialogue between patients and providers will foster a shared understanding of treatment paths that prioritize hormonal balance. With advances in research and treatment strategies, hope exists for better management solutions for those suffering from autoimmune skin diseases influenced by hormonal imbalances. Emphasizing holistic health approaches will benefit individuals, paving the way for innovative therapeutic solutions.